Contents
The vertical thickness of the soft tissue in the implant area and the volume of attached keratinized gingiva are more important than you might think. In this article, we will explore why.
How to Maintain Marginal Bone Levels: Classic Methods
Let us briefly review the common concepts for maintaining marginal bone levels. One option is the Tissue Level implant.
With this type of implant, the implant/abutment connection is located at the soft tissue level, rather than at the bone level as with Bone Level implants.
The illustration below schematically shows:
- A natural tooth
- A Tissue Level implant
- A Bone Level implant
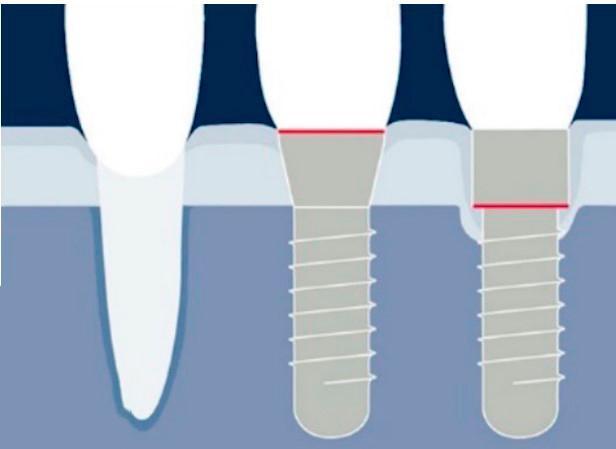
Bone remodeling diagram around different types of implants – the advantage of Tissue Level implants is shown here. YouTube/ Implantarium/ Rauf Aliyev
As shown, the gingival margin formation and marginal bone level around the Tissue Level implant are almost identical to those around a natural tooth. However, around the Bone Level implant, significant bone loss has occurred, and the gingival margin is established within the “trough” created by bone remodeling.
The reason for this is that the Tissue Level implant features a one-piece subgingival and intraosseous design. Consequently, the connective tissue attachment forms around the implant neck without necessitating bone loss.
As discussed in previous articles on soft tissue and bone healing, the soft tissue interface around an implant differs structurally and dimensionally from that of a natural tooth. The supracrestal tissue attachment (formerly biologic width) around an implant is always taller. While the normal height for a natural tooth is 2.5–2.8 mm, for an implant it is 3–3.5 mm—a difference of 0.5 to 1 mm. This is because the epithelial junction around an implant is always longer than that of a natural tooth. If the supragingival collar of a Tissue Level implant is equal in height to this soft tissue requirement (3–3.5 mm), the body has no physiological reason to resorb bone.
Moreover, with this implant type, replacing the prosthetic superstructure does not injure the deep soft tissues, removing another trigger for bone remodeling.
When Bone Level implants are placed, the soft tissue connection forms at the implant/abutment interface. Therefore, a certain amount of bone tissue is inevitably resorbed by the body to create vertical space for the supracrestal tissue attachment.
Bone loss can be minimized using double platform switching. This involves creating a mismatch at the implant/abutment interface, where the abutment base diameter is smaller than the implant platform, gradually widening toward the crown.

Microphotography of an implant and abutment using the double platform switching concept. YouTube/ Implantarium/ Rauf Aliyev
The abutment’s shoulder and concave profile create space for the soft tissue—specifically the connective tissue portion—to form precisely at the step between the implant and the abutment. A rough surface is better suited for connective tissue attachment, while a smooth surface is better for the epithelial attachment.
As a result, when platform switching is utilized, marginal bone loss is typically reduced to 0.5–0.8 mm over the first 12 months. This is slightly more than with Tissue Level implants, but clinically acceptable.
Despite the biological advantages of Tissue Level implants, they have not replaced the classic Bone Level configuration due to several factors:
- Placement is more complex and requires advanced surgical skills.
- Often, the distance between the implant platform and the opposing tooth is insufficient for the Tissue Level collar. However, Bone Level implants, combined with multi-unit V-Type abutments, allow for prosthetic restoration even in complex situations.
The illustrations below show the appearance and application principle of V-Type multi-unit abutments.
Therefore, Bone Level implants combined with screw-retained prostheses remain the “gold standard”, with modern multi-unit abutments providing solutions for complex cases.
However, almost all practicing dentists have encountered cases where even Tissue Level implants suffer 1–2 mm of bone loss, or where platform switching fails to produce the expected results. Why bone loss can sometimes be much greater than anticipated, and how to combat it, is the subject of this article.
Why Platform Switching and Tissue Level Implants Don’t Always Work
There are numerous publications demonstrating the benefits of double platform switching, yet others show little statistical difference. For a long time, there was no high-quality review explaining these discrepancies. Such studies and meta-analyses now exist.
Everything depends on the vertical soft tissue thickness. As mentioned, the peri-implant mucosa is always approximately 3–3.5 mm high. It consists of two parts:
- Connective tissue attachment: minimum 1.05 mm
- Epithelial attachment: minimum 1.88 mm
Combined, this totals roughly 3 mm. In reality, not all patients possess a soft tissue thickness of 3 mm or more above the alveolar ridge. If a patient has only 2 mm of soft tissue vertically, the body will still attempt to form a 3–3.5 mm biological seal. To achieve this, the body must resorb 1.5–2 mm of bone around the implant neck to create the necessary vertical space.
An attentive reader will ask, “Where is the evidence?” And they’ll be right: we’ll start with a classic study from the 1990s by Dr. T. Berglundh and J. Lindhe. The results of this research are now included in many textbooks.
“Dimension of the Periimplant Mucosa. Biological Width Revisited”
Briefly, the researchers placed several implants in dogs. In some cases, they raised a flap and surgically reduced the gingival thickness from 4 mm to 2 mm. The inner gingival tissue was trimmed away, leaving the mucosa intact. In the test group, the healing process was not interfered with in any way. They then observed what would happen over time.

Change in gingival thickness from 4 to 2 mm in the test group. A classic study by Dr. T. Berglundh and J. Lindhe.
After six months, they found that bone loss in the test group was nearly 1.5 mm, as shown in the illustration below. In both cases, the implants were well integrated, with healthy gingiva and a tight fit.

In the test group, bone loss averaged 1.3 mm 6 months after the intervention. A classic study by Dr. T. Berglundh and J. Lindhe. YouTube/ Implantarium/ Rauf Aliyev
The observed pattern suggests that in both cases, the body formed a supracrestal tissue attachment of 3+ mm. However, in the test group, the body had to resorb the “excess” bone to make room for it.
In the control group, the bone remained stable because there was sufficient initial soft tissue thickness.
The image below compares histological sections of the test and control groups, clearly showing the difference in bone level. However, there is virtually no difference in the shape, height, or structure of the soft tissue junction.

Comparison of histological sections of the control and test groups: in the test group, a noticeable loss of marginal bone is noted, in the control group there is no bone loss, the structure of the soft tissue connection is almost the same in both cases. A classic study by Dr. T. Berglundh and J. Lindhe. YouTube/ Implantarium/ Rauf Aliyev
The conclusion is that the level of marginal bone loss is directly related to the vertical thickness of the soft tissue at the time of surgery. But this is far from the only factor.
Back in the late 1990s and early 2000s, many researchers investigated the causes of marginal bone loss in the first year after implant placement. Specifically, this focus was on the short-term perspective; it was observed that bone remodeling processes cease after 12 months.
Several theories have been put forward. For example, Carl Misch believed that bone remodeling occurs as a result of mechanical loads.
The second popular theory was put forward by proponents of the conical implant/abutment connection. Because this connection is tighter, the so-called “bacterial pump” effect is much less pronounced. This theory suggests that the rhythmic load of chewing causes micro-movements of the abutment relative to the implant. These micro-movements cause biological fluids enriched with microflora to be pumped into the internal cavities of the interface and exit again when the cycle is repeated. It was precisely this phenomenon that was attributed to bone remodeling.

The principle of penetration of biological fluids into the internal structures of the implant. YouTube/ Implantarium/ Rauf Aliyev
This theory still has supporters, albeit they are in the minority. In reality, even a conical interface isn’t hermetically sealed enough to stop the bacterial pump effect.

Microgaps between the parts of the conical interface are still permeable to liquids enriched with microflora. YouTube/ Implantarium/ Rauf Aliyev
In fact, the conical interface makes it easier to implement double platform switching, which actually works if the soft tissue thickness above the junction is greater than 3 mm.
It would seem that these theories lead away from the real causes of the problem, which T. Berglundh and J. Lindhe had already identified. But as is often the case in science, no theory is useless. Sometimes, even an erroneous approach to testing yields a useful result. Let’s look at this in more detail.
Factors Influencing Bone Remodeling Around the Implant Neck
The dominant factor is the vertical gingival height above the bone crest. If it is less than 3 mm, bone loss is inevitable.
We discussed how and why this occurs above, based on the results of a study by Dr. T. Berglundh and J. Lindhe.
But in 2009-2010, renewed interest in this old research arose. Several new studies were conducted:
“The Influence of Soft Tissue Thickness on Crestal Bone Changes Around Implants: A 1-Year Prospective Controlled Clinical Trial” (Dr. Linkevicius et al., 2009), published in International Journal of Oral & Maxillofacial Implants
Dr. Linkevicius’s group set the task of examining how the loss of marginal bone around the implant is related to the initial gingival thickness above the alveolar ridge. They placed identical implants in all patients and measured the gingival height during the operation.
And this is what they found:
Bone loss was directly related to gingival thickness, which replicates the findings of T. Berglundh and J. Lindhe’s group.
The x-rays below show the condition of the bone around implants with an initial gingival thickness of ≥2.5 mm. The left image shows the bone condition at the time of implant placement, and the right image shows it 12 months after implantation. As you can see, the marginal bone condition has remained virtually unchanged.

The condition of the bone at the time of placement (left) and after 12 months (right), provided that the level of soft tissue above the bone is ≥ 2.5 mm – the level of the marginal bone is preserved. YouTube/ Implantarium/ Rauf Aliyev
In the following images, the gingival thickness above the ridge was less than 2 mm. On the right slide, after 12 months, there is already noticeable bone loss around the neck of the implant.

The condition of the bone at the time of placement (left) and after 12 months (right), provided that the level of soft tissue above the bone is 2 mm – after 12 months, a decrease in the level of the marginal bone was noted. YouTube/ Implantarium/ Rauf Aliyev
Let’s move on to the next study.
“Influence of Thin Mucosal Tissues on Crestal Bone Stability Around Implants With Platform Switching: A 1-year Pilot Study” (Dr. Linkevicius et al., 2010), published in Journal of Oral and Maxillofacial Surgery
This in vivo study from the same group shows a link between initial gingival level and the platform switching concept.
Volunteers had two identical implants placed side by side and, if possible, at the same level relative to the bone. The only difference was that one had a platform switch, while the other did not (see photo below).

Implant placement without platform switching (left) and with platform switching (right) – the goal is to determine the difference in marginal bone loss. YouTube/ Implantarium/ Rauf Aliyev
The initial gingival height was measured during the soft tissue dissection stage. The difference is visible in the image below. The top slide shows very thin gingiva, while the bottom slide shows much thicker gingiva.
The group with thin gingiva included patients whose soft tissue thickness was 2 mm or less, and the group with thick gingiva included patients whose thickness was more than 2 mm.

Measurements of the thickness of the gingiva above the alveolar ridge: upper image – thickness <2 mm; lower image – thickness >3 mm (almost 5 mm). YouTube/ Implantarium/ Rauf Aliyev
The results confirmed the research team’s hypothesis that the effectiveness of platform switching is directly related to the thickness of the original gingiva.
Here’s an X-ray of one of the patients in the thin gingiva group. The left image shows the bone level at the time of implant placement, and it’s clear that both implants are positioned at bone level. The right image was taken 12 months later, and it shows that bone remodeling has occurred, and the necks of both implants were exposed. Moreover, the level of bone loss was almost the same for both platform-switching and non-platform-switched implants. Whereas in the group of patients with gingival thickness greater than 2 mm, bone loss around implants with platform switching was noticeably less.

X-rays of the same patient: bone level around implants at the time of placement (left) and after 12 months (right), the right image shows noticeable and almost equal bone loss around both implants. YouTube/ Implantarium/ Rauf Aliyev
This and other works became the foundation for systematizing data on the problem of preserving both bone and soft tissue. The result was a book “Zero Bone Loss Concepts” (First edition, 2019). This book is already known to many practicing dentists, but not all have read it. That’s why we’re so interested in the key concepts in this book.
Let’s move on to the practical conclusions that can be drawn from the aforementioned studies and this book.
How to Maintain the Highest Possible Bone Level: The “Zero Bone Loss” Concept
The following is a list of factors that determine the remodeling of marginal bone around the neck of the implant. This applies to both Tissue Level and Bone Level implants, but with some nuances that will be highlighted separately.
- Distance from the bone edge to the internal border of the implant/abutment joint.
The further this border is from the bone surface, the less resorption occurs, and here Tissue Level implants have a clear advantage. However, this is a universal rule: if a Tissue Level implant is placed at bone level, the bone remodeling pattern will be the same as with a Bone Level implant.It is important to clarify the meaning of placing implants below the level of the bone, the so-called subcrestal placement. If a patient has a thin layer of gingival tissue above the bone, the doctor understands that bone loss is inevitable. In this case, the implant is immediately placed 1.5-2 mm below the bone level, which seems counterintuitive. But the rationale becomes clear when, after a few months, bone remodeling occurs. Yes, as we’ve already established, the body removes some bone tissue to form the gingival cuff. But in the case of subcrestal placement, the implant neck is not exposed. The area of bone contact with the implant remains the same. - Initial gingival thickness above the alveolar ridge. Let’s look at another case. The images below show a Tissue Level implant. On the left is the bone condition at the time of implant placement with a healing cap; on the right, approximately one year after placement.

The condition of the marginal bone: at the time of placement of the healing cap (left); 12 months after implant placement (right). The second image shows a noticeable loss of bone level; this is due to the initially thin gingiva above the alveolar ridge. YouTube/ Implantarium/ Rauf Aliyev
The right slide also shows that the marginal bone level has decreased. This isn’t critical, and this restoration will last a very long time. However, this case is 100% consistent with the results of the studies mentioned above. This patient’s initial gingival height was just over 2 mm. Bone remodeling is inevitable, which is what we see in the picture. For this type of implant, a gingival thickness of 3 mm is required to avoid bone remodeling.
Now let’s look at another case and see what happens when Bone Level implants are used. Note the amount of attached gingival tissue in the completely edentulous jaw. The gingival tissue is thick and massive, which is a good sign.

Initial condition of the jaw with complete edentia, visual assessment: wide alveolar ridge, thick attached keratinized gingiva. YouTube/ Implantology/ Rauf Aliyev
It’s worth remembering that the quality of the soft tissue connection around an implant is inferior to that around a natural tooth. The only thing that can compensate for this loss of soft tissue connection quality is a large volume of attached keratinized gingiva. This acts as a mechanical damper, preventing the gingiva from retracting. The gingival cuff remains stable and dense, which means the risk of peri-implant mucositis and peri-implantitis is minimized.
So, at first glance, this patient’s outlook appears excellent. But during the surgery, this is what we see:

During the operation, it was discovered that the thickness of the soft tissue above the ridge ranged from 1.5 to 2 mm in different areas. YouTube/ Implantarium/ Rauf Aliyev
If you look at the palatal portion of the flap, you’ll see that it’s quite thin—about 2 mm or even slightly less. On the vestibular side, the flap is even thinner, about 1.5 mm.It turns out that at the initial examination, we see a wide alveolar ridge and a thick layer of attached gingiva—all of which is fine—but the soft tissue layer is vertically thin. This means that bone loss is inevitable.
IMPORTANT! Let’s digress to remind you about gingival phenotypes. These are innate characteristics of the body that even correlate with a person’s appearance.

Common tooth shape variations associated with different amounts of keratinized attached gingiva: an elongated shape with high zeniths is most often associated with a thin layer of attached gingiva, while a square profile is associated with a thick phenotype. YouTube/ Implantarium/ Rauf Aliyev
If a person has a thin and graceful build, he will most likely have elongated teeth and the so-called thin-scalloped phenotype. This phenotype is characterized by long papillae and a relatively thin layer of attached gingiva. Conversely, if a person naturally has broad shoulders, thick hands, and a strong jaw, the gingival contour will likely be smoother, the teeth will appear square, and the attached gingiva will be thick and wide. The second type tolerates implant placement much better, and the complication rate is much lower.
There is a simple way to check the thickness of the attached gingiva using a regular probe.

Checking the gingival biotype (thickness of attached gingiva): on the left, the probe is translucent and clearly visible through the gingiva – a sign of a thin biotype; on the right, the probe is poorly visible – a sign of a thick biotype. YouTube/ Implantarium/ Rauf Aliyev
If the tip of the probe is clearly visible through the gingiva, it is closer to the thin phenotype; if it is almost invisible, then it is thick.
But in reality, extreme cases are almost never encountered, as this clinical case confirms. Furthermore, it is possible to increase the thickness of attached gingiva, that is, change the phenotype, through soft tissue grafting. Therefore, the term “biotype” has been abandoned in favor of “phenotype,” because “biotype” implies something fundamentally inherent in nature and cannot be changed.

An example of increasing the thickness of attached gingiva using soft tissue plastic surgery. YouTube/ Implantarium/ Rauf Aliyev
Let’s return to our case: the patient has been toothless for a long time and it is difficult to judge what the thickness of the gingiva was before.
Currently, a number of positive factors are observed: a wide ridge and massive attached gingiva, but also a negative factor – too thin a layer of soft tissue above the alveolar ridge.
The next photo is from the abutment try-in stage. From the frontal view, a strong band of attached gingiva is visible, which is excellent. This means the soft tissue connection will be stable and protected from mechanical stress during chewing.
And from this angle, we see that the alveolar ridge is wide and there is sufficient bone reserve on both the palatal and vestibular sides. And this is also very good.
But if you compare three x-rays:
- Immediately after implantation
- In 3 months
- After 12 months…you can see changes in the level of the marginal bone.
…you can see changes in the level of the marginal bone.
X-rays: immediately after implantation, 3 months and 12 months after implantation. YouTube/ Implantarium/ Rauf Aliyev
In summary, this “pure experiment” case demonstrates that the initial gingival thickness is the decisive factor for bone remodeling. Despite other positive factors such as:
- Broad alveolar ridge
- Good volume of keratinized attached gingiva
- Double platform switchingThe outlook for this restoration is still good, the formation of the gingival junction is complete, and the remaining bone contact is sufficient for implant stability, as the risk of gingival recession is minimal. However, if the patient has other negative factors, a loss of 1-2 mm of marginal bone can be critical for implant survival.
- Attachment trauma due to replacement of superstructures. This includes the placement of a healing cap several weeks after implantation, multiple abutment replacements during the fitting period, etc. All of this interferes with the formation of a soft-tissue connection, and each trauma stimulates cuff growth. Consequently, the body resorbs additional bone tissue. There are two ways to circumvent this::
- Use Tissue Level implants, which is obvious, because the superstructure is located above the gingival level.
- Use multi-unit abutments for screw retention with Bone Level implants, such as the MUA V-Type.

The principle of fixing a prosthesis on a multi-unit abutment – a schematic example is shown. MUAs are used only for multiple restorations; for single ones other types of abutments are provided. YouTube/ Implantarium/ Rauf Aliyev
Multi-unit abutments are placed immediately after implantation, or at the same time as the healing caps, and remain in place for the remainder of the prosthesis’s lifespan. This reduces gingival trauma, thereby maintaining gingival height.
How to Use the Data in This Article in Practice
It’s time to move on to practical conclusions.
- The relationship between bone loss and the position of the implant/abutment interface. Another interesting study is worth mentioning: Peri-implant Inflammation Defined by the Implant-Abutment Interface. We found that the lower the platform and the implant/abutment connection, the greater the bone loss, and this is confirmed by the results of this study (see the illustration below).

Bone loss with different implant placement methods, but other conditions being the same: minimal loss is observed with supracrestal placement, which is logical and confirmed by other studies; maximum bone loss is observed with subcrestal placement. YouTube/ Implantarium/ Rauf Aliyev
This is due to the fact that the connective tissue connection always forms below the implant/abutment line, so bone remodeling occurs to a greater extent than with other schemes. But as we mentioned earlier, subcrestal placement maintains implant stability when the soft tissue thickness above the alveolar ridge is less than 2 mm. In this case, tissue remodeling still occurs to create a 3-3.5 mm gingival cuff, but the implant neck is not exposed.
- The condition of the implant neck surface. Connective tissue plays a key role in the formation of the gingival cuff. Fibrin fibers adhere better and more easily to irregularities, resulting in faster and more compact soft tissue adhesion. Consequently, bone loss will be reduced. Currently, the surface of 100% of implants is modified in some way. However, there is a significant difference in processing technologies. The images below show the results of different surface processing methods under a microscope.

The central slide shows the surface of XGate implants treated with the proprietary Pure & Porous (P& P) technology. It combines the best of both SLA and RBM technologies. The problem is that SLA (a hard abrasive made of aluminum oxide and acid etching) produces an excellent relief, but it is very difficult to remove all impurities and abrasive fragments. RBM technology uses a biocompatible hydroxyapatite abrasive and eliminates the problem of aggressive impurities. However, it is a very soft material and cannot create the same deep relief as aluminum oxide.The surface of XGate implants is quite textured and close to the surface obtained using SLA technology, and is as clean as possible from impurities, which is typical for RBM technology (see the illustration below).
SEM BC microphotographs at magnification 50 presents dental implants of: XGate Dental (image 1), one of worldwide leaders in the field (image 2) and a well-known manufacturer (image 3).
XGate implants demonstrate surface cleanliness equal to the worldwide leader in the field.
- All the processes mentioned in this article, as well as the methods for counteracting bone loss, are only relevant during the first few months, up to a year at the most. If the load on the restoration is uniform and everything is functioning optimally, then after 12 months, the bone level stabilizes. And here, the amount of attached keratinized gingiva becomes paramount.

An example of a good thickness of attached gingiva, which gives a favorable prognosis in the long term. YouTube/ Implantarium/ Rauf Aliyev
The following illustration clearly shows that healthy gingiva completely compensates for bone loss around the implant.
If the attached gingiva is insufficient, many specialists perform gingival grafting simultaneously with implant placement. Both the apically displaced flap and free graft techniques are widely used. This is critical for long-term success.
We hope this article was interesting and that XGate Dental products will help improve your implant success rates. Stay tuned for our next publications.
Disclaimer: Any medical or scientific information provided in connection with the content presented here makes no claim to completeness and the topicality, accuracy and balance of such information provided is not guaranteed. The information provided by XGATE Dental Group GmbH does not constitute medical advice or recommendation and is in no way a substitute for professional advice from a physician, dentist or other healthcare professional and must not be used as a basis for diagnosis or for selecting, starting, changing or stopping medical treatment.
Physicians, dentists and other healthcare professionals are solely responsible for the individual medical assessment of each case and for their medical decisions, selection and application of diagnostic methods, medical protocols, treatments and products.
XGATE Dental Group GmbH does not accept any liability for any inconvenience or damage resulting from the use of the content and information presented here. Products or treatments shown may not be available in all countries and different information may apply in different countries. For country-specific information please refer to our customer service or a distributor or partner of XGATE Dental Group GmbH in your region.