Contents
In this section, we will continue to examine the criteria for selecting implants and abutments, determine how many implants are needed per jaw, and detail the proper implant positioning for the Full Arch on 4/6 protocol.
Selection and Positioning of Dental Implants
Full-arch implant-supported prosthetics involve numerous nuances, including implant design, surgical site preparation, and angulation. Unfortunately, not all clinicians are willing to delve into these “minor details,” yet this is the only way to consistently achieve high-quality restorations that remain successful for 10, 15, or more years.
In the previous section, we concluded by examining the differences between implants designed for cortical bone versus cancellous bone and which designs suit different bone densities (D1 to D4). In this part, we will start with implant diameter. The table below, based on the Carl Misch classification, is considered a standard reference.
| Classification | Diameter, mm | Purpose |
|---|---|---|
| Small | 3.0–3.75 | Lower incisors, upper lateral incisors |
| Average | 4.0–4.5 | Medial maxillary incisors, canines, premolars |
| Big | 5 or more | Molars |
However, this is not a rigid canon; there are clinical cases where these recommendations must be adapted. For example, 4.0–4.5 mm diameter implants can be placed in molar positions if the alveolar ridge width precludes a 5.0 mm implant. As a reminder, the thickness of the buccal bone wall must be at least 2 mm. Otherwise, bone loss in both height and thickness on the buccal aspect is inevitable. It is better to place an additional, smaller-diameter implant or maintain the same number of implants but of a smaller diameter than to compromise the crestal bone.
Implant length is the next criterion, with its own specific classification:
| Designation | Length, mm |
|---|---|
| Standard | 10 mm or more |
| Short | 7–8 |
| Ultra-short | 6 or less |
There are now other classifications; for example, data from a consensus conference recommends calling implants 6 mm or less in length “short,” and considering the rest as “standard.”
There are numerous studies confirming that short implants are almost as effective as standard ones, because the upper 5–6 threads bear the main load. However, we won’t go into detail about this, as the topic of this article is full-arch prosthetics supported by 4/6 implants, and ultra-short implants are not used in this protocol. However, non-standard options are possible.
For example, four standard-length implants and two short ones in the distal sections can be used to avoid long cantilevers. A full arch on implants is a mechanically complex structure, and when loaded in the distal sections, the anterior implants experience a tensile load. Therefore, long cantilevers (more than 10 mm) are highly undesirable, but a cantilever length of 14 mm is considered the maximum.
But let’s return to the standard protocol for full-arch prosthetics on 4/6 implants. To ensure that the structure is mechanically stable, it is necessary that:
- The length of the implants is not less than 11 mm
- The diameter is not less than 3.75 mm
This relatively long length is due to the average height of a fixed bridge on implants, including abutments, being 5–7 mm. If the length of the superstructure is commensurate with the length of the implant, achieving stability is very difficult. Sooner or later, chewing forces will loosen the implant. The height of the prosthetic structure can be as high as 10–12 mm, so a minimum length of 11 mm is recommended, and the length of angled implants can be even greater.
Mechanical stability of the implant is crucial; if it is lost due to mechanical overload, a cavity forms around it and significant bone volume is lost.
Reimplantation is therefore impossible without extensive bone grafting. Of course, there are exceptions, as the patient could be a tall man with strong jaws or a petite woman. Jaw sizes, the space available for implants, and consequently crowns, can vary. Some people need 15 mm implants, while others can use 10 mm. If the jaw anatomy does not allow for implants of sufficient length, this can be compensated for by adjusting the implant diameter. The bone-titanium contact area will remain the same, ensuring stability. Alternatively, increase the number of implants, for example, not 4, but 5 or 6.
The question may arise: how to determine the height of the prosthetic structure in advance? This is calculated during the surgical planning stage. It is crucial to take an initial impression while the patient still has the teeth or bridges to be removed. Quite often, such an impression is used to fabricate a temporary prosthesis on-site (without a dental laboratory). Of course, CBCT data and 3D modeling of the prosthesis, as well as the positioning of the implant placement points, will help with this.
Let’s return to the photo from the previous part.
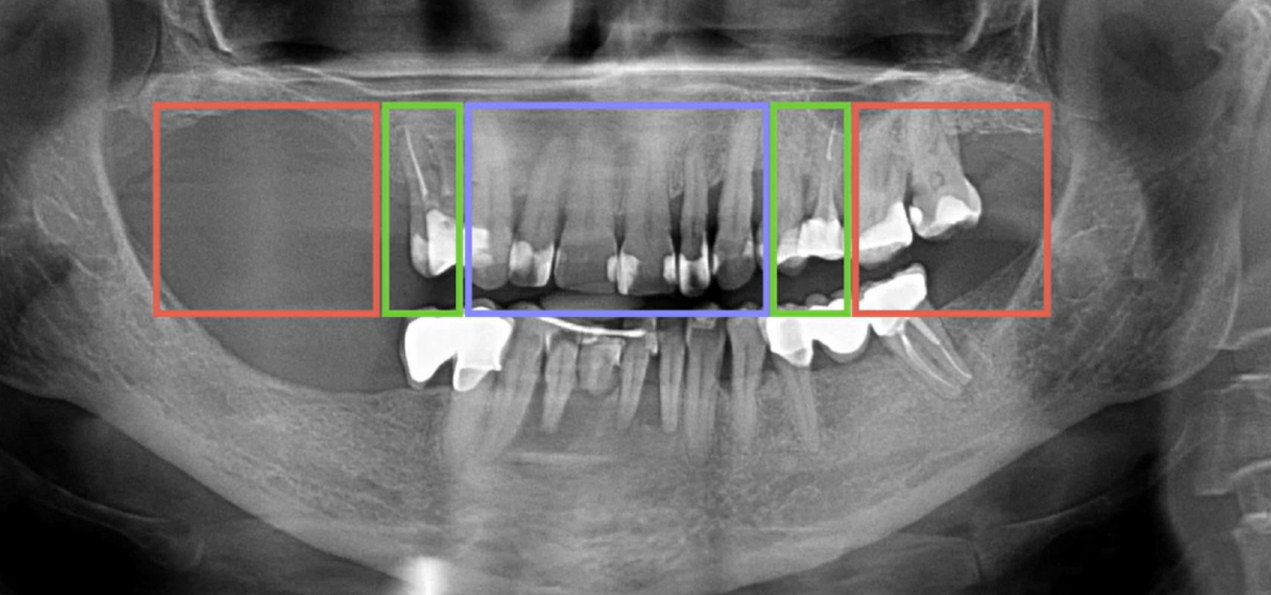
initial orthopantomogram of the patient. Full-arch prosthetics with support on implants is planned. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
Here you can see the height of the teeth and the changes in the bone tissue that will need to be addressed. Of course, in most cases, the original occlusion should be maintained and the bite should not be “played with.” In this clinical case, the alveolar process will need to be leveled and some bone will need to be trimmed in the incisor area. Therefore, it’s easy to assume that the height of the prosthetic structure with abutments will be quite large.
The minimum implant diameter is related to the wall thickness at the implant/abutment interface. This is because the diameter of the conical interface where the abutment is inserted into the implant is the same for all implant diameters, and it’s important that the wall thickness withstands lateral and axial loads. After all, if the entire jaw is supported by four implants, the load on each one is significantly greater than with a protocol that uses 8–10 implants for the entire jaw. And with an implant diameter of 3.75 mm, the wall thickness is just over 0.5 mm. Of course, titanium is a very strong metal, but if the part is made too thin, it won’t withstand the load. Titanium-vanadium-aluminum alloys of Grade 5 and Grade 23 offer some protection against implant wall cracks, but if the wall thickness is less than 0.4 mm, the risk of implant fracture is very high. However, this only applies to immediate implant restorations using the Full Arch on 4/6 protocol. For other protocols with a larger number of implants, thinner implants can be used.

XGate Dental implant with conical interface in cross-section – multi-unit V-type abutment shown as an example.
What is Total Insertion Torque and Why is It Important for Immediate Loading of Implants?
Total insertion torque is the most immediate, although indirect, criterion for assessing primary implant stability. General implantology uses a classification system; see the table below.
| Torque, N·cm | Actions for Immediate Loading | Notes |
|---|---|---|
| More than 50 | Replace the implant by under-preparing the osteotomy slightly; otherwise, there is a high risk of bone necrosis and loss of stability. | An exception is if a cancellous implant with wide-pitch threads is placed in D4 bone. |
| 35–40 | Ideal indicator, can be loaded without restrictions. | — |
| 20–25 | Insufficient for single implantations, but acceptable if the total insertion torque is within normal limits. | If other implants on which the prosthesis rests have a higher torque and the total torque for 4 implants is at least 120 N·cm. |
| 15 or less | Cannot be used. | It can be replaced with an implant of a larger diameter and with a different thread profile. |
Surgical Trauma and Implant Macrodesign
In the previous section, we discussed thread shape and bone density. The key point is conical implants with wide, aggressive threads for low-density D3-D4 bone, and cylindrical implants with fine, smooth threads for dense D1-D2 bone. However, not every dentist is willing to order highly specialized implants when there is a way to place standard ones without compromising stability.
For example, XGate Dental implants with a variable thread profile offer an interesting solution.
And yes, such implants allow achieving sufficient primary stability in both dense D1 and soft D4 bone. However, the protocol for full-arch restoration using 4/6 implants imposes its own limitations. There are few implants, and each one carries a significant load, especially in the distal regions. And if the bone density is low, this can be a problem. A solution in this situation is to compact the osteotomy walls using osteotomes. This instrument compresses the trabeculae and compacts the bed walls, rather than extracting bone fragments like a drill. This treatment can improve the primary stability of the implant, which is critical.
Distant and Contact Osteogenesis
Let’s return once again to the topic of choosing the right implants for cancellous and cortical bone. If for some reason the surgeon installs an implant with wide, aggressive threads in dense bone, it’s a poor decision. To screw such an implant into dense bone, the osteotomy will have to be widened, and only the tips of the threads will be in contact with the bone. Significant cavities will form between the implant body and the bone. There’s a high risk of osseointegration failure. The bone tissue won’t fuse to the titanium as it should, and a bone wall will form at the edge of the implant bed. Clearly, sufficient implant stability is out of the question. A cortical implant placed in D3-D4 bone is the opposite option. The thread profile is low, the distance between the threads is small, and the trabeculae are large, making the bone porous. This also prevents proper contact between the titanium and the bone.
In this scenario, achieving both primary and secondary stability is difficult. While secondary stability may be sufficient when replacing a small bridge using a two-stage protocol, it is not so with a full arch 4/6.

Diagram of osseointegration failure due to incorrect implant design selection. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
Immediate implantation, especially with immediate loading, often requires placing implants in the socket of an extracted tooth (see photo below). This can lead to bone deficiency and low density, especially in the upper jaw.

An example of a socket from an extracted tooth with an inter-root septum where the implant will be placed. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
And to ensure primary stability in such conditions, there are two options:
- Use cancellous implants with wide-pitch threads that will penetrate deep into the bone
- Compact the bone tissue in the area of the osteotomy using osteotomes and apply a universal implant.
Positioning and Stabilization of Implants
Now, we won’t discuss positioning from an orthopedic perspective. First, let’s consider positioning and stabilization, taking into account anatomical features and bone volume.
- Vertical positioning. Here it is necessary to take into account anatomical features.
If it’s the upper jaw, the implant’s apex may penetrate the maxillary sinus. If it’s 2-3 mm, sinus lifting is generally not necessary. The main thing is that the bone thickness is sufficient to secure the implant. Standards and indications for sinus lift are a separate topic, so we won’t discuss it in detail.The lower jaw is at risk of damaging the mandibular nerve or artery.In any case, you should not make mistakes like those in the illustrations below.
Errors in vertical implant positioning: on the left, the implant is too deep, significantly below the crestal bone level, which is why the socket of the extracted tooth did not heal completely; on the right, the implant is too long, almost passing through the jaw. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
- Positioning by width. At the 2023 ITI Consensus Conference, it was announced that the thickness of the buccal bone wall should be no less than 1.5 mm, with 2 mm considered the “gold standard.” However, meeting this requirement is not so straightforward when an implant needs to be placed in a socket following the extraction of a multi-rooted tooth. Here, careful surgical planning becomes paramount, and the use of a surgical template is one option.

A plan to place an implant in the socket of a recently extracted tooth. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
Also suitable for such cases are implants with wide, aggressive threads and a large diameter of 5-6 mm, because the volume of bone required to stabilize the implant is very small.
- Rules for implant positioning in the lower jaw. Unless there are special conditions or restrictions, the Full Arch on 4 design typically places implants in the 3 and 6 tooth positions, while maintaining occlusion keys.

Basic implant placement scheme for the Full Arch on 4 in the lower jaw. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
However, doctors often encounter bone deficiency in the posterior regions, which shifts the formula slightly and implants are placed in the 2 and 5 tooth positions. This is slightly worse, but it is still possible to create a 12-tooth prosthesis, provided the basic rules are followed:
- The distance between implants is 1.5-2 cm
- The length of the distal cantilevers does not exceed 14 mm
The number of implants is not a rigid requirement. If, with a classic placement for teeth 3 and 6, the distance between the implants significantly exceeds 2 cm, the number of implants can be increased, for example, by placing one in the center. This may be the case for patients with a very large frame.

Diagram of implant placement with an additional unit in the center for large patients when the distance between the implants at the canine positions exceeds 20 mm. YouTube/ Dr. Sergey Rozhnov /sergiodontolog
And here’s what it looks like in reality: the photo below shows the patient’s lower jaw with classic direct implant placement.

Clinical example of four implants placed in the lower jaw. YouTube/Dr. Sergey Rozhnov /sergiodontolog
Another common solution for bone deficiency in the posterior region is the placement of angled distal implants. This is becoming more of a standard, not only for cases where even the fifth tooth position cannot accommodate straight implants, but also for moderate bone deficiency. Angled implant placement allows the prosthetic platform to be positioned at the sixth tooth position, with the implant apex positioned in the fourth tooth area. Furthermore, this results in a long implant with a good bone-titanium contact area.
Yes, an angled abutment and screw will experience greater load than a straight one, but this is usually justified. Reducing the length of the cantilevers is always biomechanically beneficial. The risk of screw loosening or breaking on an angled implant is significantly higher. However, replacing a broken screw is easier than dealing with a broken prosthesis or implant lost due to loosening caused by the cantilever load.
The illustration below shows the design of the D-type angled abutment from XGate Dental.
Thanks to high manufacturing precision, the implant-abutment connection remains stable even under significant stress caused by the deviation of the loading axis from the implant axis.
The risk of fixation screw fracture is also minimized thanks to the Grade 23 alloy, which offers a higher degree of elastic deformation compared to pure titanium.
The standard is considered to be MUA with angles of 17°, 30° and 45°, which allow for compensation of implant deviation from 74° to 130° (see illustration below).
Slight implant angulations (up to 40°) can be compensated even by straight V-type abutments.
This is possible due to their very low interface profile, where the short taper and compact cylinder allow compensating for divergences of up to 40°.
As a result, the prosthesis remains fully functional.
- Guidelines for implant positioning in the upper jaw. It’s best to place six implants in positions 2, 4, and 6.

An example of optimal implant positioning in the upper jaw. YouTube/Dr. Sergey Rozhnov /sergiodontolog
But if there is a deficiency of bone tissue in the distal sections, which is typical for the upper jaw, then displacement in the positions of teeth 1, 3, 5 is allowed.
If the patient is petite, four implants in positions 2 and 5 may be sufficient. In some cases, as with the lower jaw, a single implant can be placed centrally to provide five points of support. However, it should be noted that, unlike the lower jaw, the upper jaw has a Sutura intermaxillaris, which remains mobile throughout life in many patients. Therefore, placing the implant precisely in the center between the central incisors is not recommended. A formula of 1, 3, 5 in one quadrant and 3, 5 in the other can be used.
The 3.6 formula is rarely used for the upper jaw. The upper jaw is always wider, and the distance between implants would be too large.
If there is a significant bone deficiency in the maxillary sinus area or the budget prohibits sinus lift surgery in the upper jaw, implants are also placed at an angle. The principle is the same as for the lower jaw, including the use of angled multi-unit abutments.
We won’t discuss the specifics of using zygomatic implants or implant tilting with tuberosity support in this article, as this is a complex procedure. Full Arch on 4/6 protocols are budget-friendly and often offer special offers. The Full Arch on 4/6 protocol is marketed as a single-day implantation and prosthetic procedure, which is not possible with zygomatic implants.
That’s all for now. In the next section, we’ll discuss the choice of multi-unit abutments and why Full Arch on 4/6 protocols use only screw retention. We’ll also discuss methods for fabricating both simple and laboratory-made temporary prostheses.
Stay tuned for our next publication.
Disclaimer: Any medical or scientific information provided in connection with the content presented here makes no claim to completeness and the topicality, accuracy and balance of such information provided is not guaranteed. The information provided by XGATE Dental Group GmbH does not constitute medical advice or recommendation and is in no way a substitute for professional advice from a physician, dentist or other healthcare professional and must not be used as a basis for diagnosis or for selecting, starting, changing or stopping medical treatment.
Physicians, dentists and other healthcare professionals are solely responsible for the individual medical assessment of each case and for their medical decisions, selection and application of diagnostic methods, medical protocols, treatments and products.
XGATE Dental Group GmbH does not accept any liability for any inconvenience or damage resulting from the use of the content and information presented here. Products or treatments shown may not be available in all countries and different information may apply in different countries. For country-specific information please refer to our customer service or a distributor or partner of XGATE Dental Group GmbH in your region.
